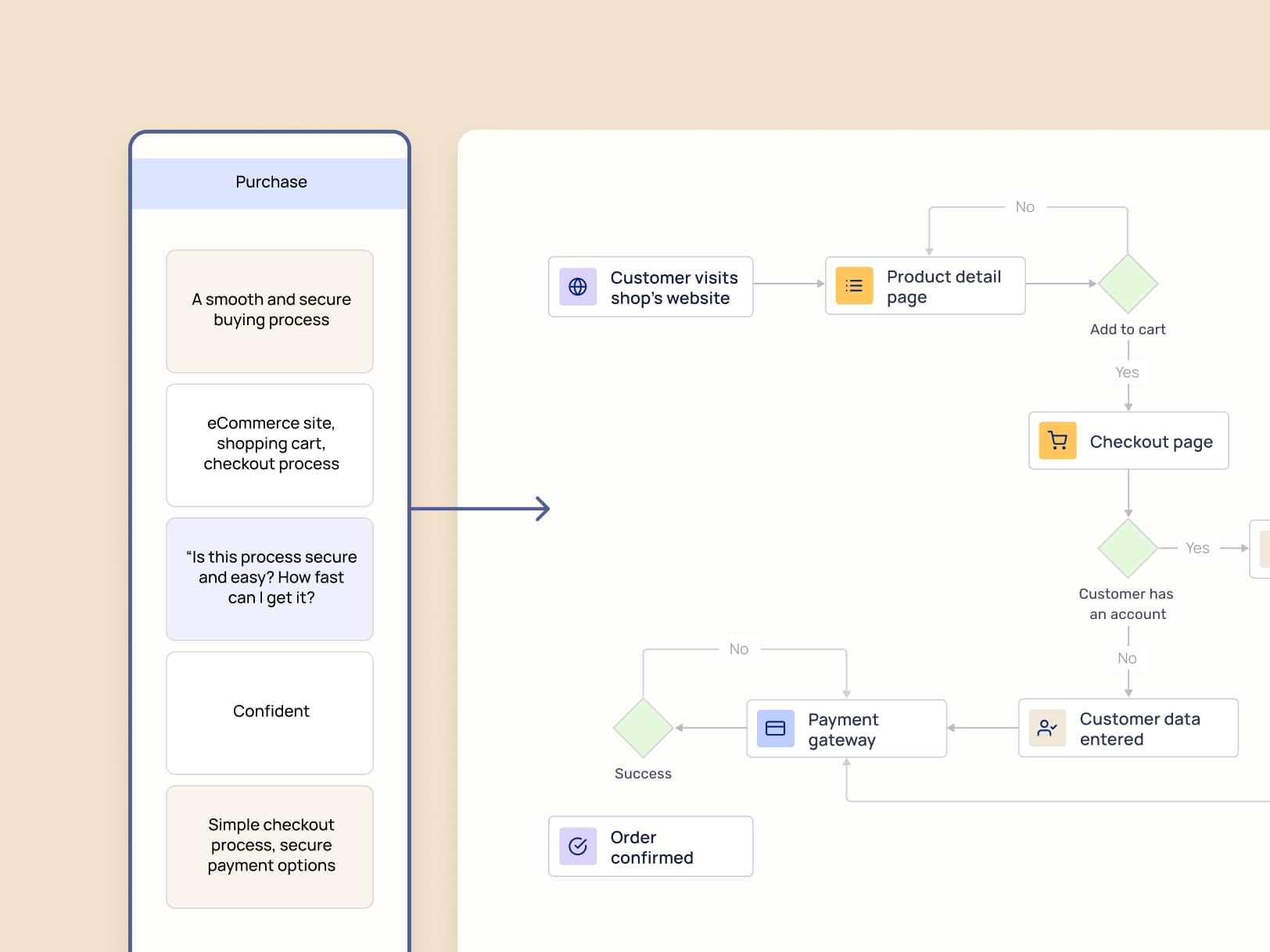
Every insurance leader we speak with has the same conversation: AI is a priority, experiments are running, and the results are underwhelming relative to the investment of time and attention. This article is an attempt to explain why — drawing on the latest research from McKinsey, BCG, and MIT — and to give regional carriers a clear-eyed picture of where the real returns are, what's holding most teams back, and what the path from experimentation to operational advantage actually looks like.
The adoption surge — and the performance gap hiding inside it
.jpg)
Insurance has quietly become one of the most aggressive AI adopters of any industry. A 2024 BCG survey found insurance companies outpacing nearly all other sectors in AI adoption — reaching near-parity with technology and telecommunications firms, a remarkable shift for an industry that spent decades as a digital laggard.
The performance data is equally striking. McKinsey's 2025 analysis identifies a small cohort of AI-forward insurers that have generated 6.1 times the total shareholder return of their lagging peers over five years — a performance spread wider than in almost any other industry.
But headline adoption numbers conceal a more complicated reality. Only 7% of insurance companies have successfully brought AI to scale. About two-thirds of insurers are still in the piloting stage, according to BCG's Build for the Future 2024 Global Study. The gap between experimenting with AI and systematically operationalizing it is where the real competitive story is being written — and understanding it requires looking honestly at where AI is actually delivering results, not just where it's generating executive enthusiasm.
Where the returns are real
Claims processing
Claims processing is the most mature AI application in insurance, and the performance data is substantial. Industry analysis puts overall claims resolution time reductions at up to 75% at AI-enabled carriers — with routine claims dropping from 7–10 days to 24–48 hours. (Datagrid, 2025)
These are not projections. Aviva deployed more than 80 AI models across its claims domain, cutting liability assessment time for complex cases by 23 days, improving routing accuracy by 30%, and reducing customer complaints by 65% — saving the company more than £60 million in 2024 alone. (McKinsey)
The mechanism is straightforward. AI handles first notice of loss intake, document extraction, initial triage, and coverage verification — the high-volume, rule-based work that consumes experienced adjusters' time without requiring their judgment. When those steps are automated or AI-assisted, adjusters direct their expertise toward what genuinely demands it: complex coverage disputes, contested liability, and the contextual judgment that no model replaces.
Underwriting
Underwriting is where the growth trajectory is steepest. AI adoption in underwriting sits at 14% today but is projected to reach 70% by 2028 — the highest growth rate of any insurance function. (Datagrid, 2025)
The efficiency case is compelling even at modest scale. Manual submission processing for a commercial lines account typically takes 15–25 minutes — extracting data from broker emails, normalizing it, entering it into systems, identifying gaps. AI-assisted extraction brings that to under two minutes. For a team handling 20 new submissions per week, that's 4–8 hours recovered per underwriter, every week, without changing a single underlying system.
McKinsey notes that in selected commercial lines cases, quoting times have been reduced from several weeks to days, and in some instances from multiple days to just a few hours.
Fraud detection
Fraud detection has the highest current adoption rates among AI use cases in insurance, with industry analysis suggesting reductions in fraud losses of 20% or more at carriers using AI-powered detection systems. (Datagrid, AllAboutAI)
This is one area where proprietary models trained on a carrier's own claims history genuinely matter. But it is also the exception. For the operational workflows that consume the most time across underwriting, claims, and policy servicing, proprietary AI is not the differentiator most carriers assume it is.
The tool question: access is not the advantage
One of the most persistent and costly misconceptions in insurance AI is that competitive advantage requires building or buying specialized insurance-specific tools. The data doesn't support this.
76% of insurance companies have implemented generative AI in at least one business function as of mid-2024 — the majority using general-purpose tools: ChatGPT, Claude, and Gemini. Access to capable AI is no longer a differentiator. It's a baseline.
Leading insurers achieve loss ratios that are, on average, six percentage points better than their competitors, and are nearly twice as likely to have prioritized significant investment in their underwriting operations. The advantage is not in which AI vendor they use. It's in how deeply AI is embedded into the way they actually work.
McKinsey is direct on this point: getting AI transformation right requires fundamentally rewiring how an organization operates — embedding technology into intake, triage, underwriting, and claims workflows at the process level, not deploying it as a parallel tool that sits beside existing operations and depends on individuals remembering to use it.
.jpg)
The integration problem: where most value is still being left behind
Here is an honest description of where most insurance teams using AI actually are today.
A broker email arrives. Someone opens ChatGPT, pastes in a well-crafted prompt, receives a clean structured data table, and then manually copies that output into their policy admin system or CRM. The result is genuinely better than what they had before. But a human is still performing a data transfer step that adds no analytical value, introduces error, and doesn't scale.
MIT's 2025 study The GenAI Divide found that 95% of enterprise AI pilots delivered no measurable P&L impact — with integration gaps, governance failures, and disconnected operating models cited as the primary causes. The bottleneck isn't the AI. It's the disconnection between what AI produces and the systems that need to act on it.
McKinsey identifies change management as the decisive differentiator between AI sitting idle and AI genuinely transforming operations. Having excellent technology is only half the battle. The other half is embedding AI into daily tasks in a way that actually shifts how work gets done.
That shift requires two things operating in concert:
- Prompting discipline — structured, documented workflows that ensure AI is used consistently across a team, not just by the few individuals who've developed reliable practices on their own
- Integration — connecting AI output directly to the systems your operation already runs on, so that output doesn't become another manual processing step
Most carriers have made meaningful progress on the first. Almost none have fully solved the second.
Where EasySend fits in
This is precisely the problem EasySend was built to close. We work with insurers every day on the operational challenge this article describes — the gap between AI producing the right output and that output being where it needs to be, without a human manually bridging the two.
Our platform digitizes the intake forms, submission workflows, claims processes, and agent portals that currently run on PDFs and email — with AI extraction and routing built directly into the operational flow. When a broker submits an application through an EasySend-powered journey, the data doesn't arrive in a shared inbox waiting to be processed. It enters a digital workflow, gets extracted and structured automatically, and routes to your underwriting queue, CRM, or policy admin system — without a manual step in between.
The same logic applies across claims intake, policy servicing, endorsement requests, and agent onboarding.
The carriers we work with aren't replacing their core systems to achieve this. They're adding an intelligent workflow layer that sits between the outside world and their existing technology — one that typically goes live in weeks, requires no large IT project, and doesn't depend on a transformation budget to implement.
The prompting techniques we've shared in our AI playbook build the first layer: consistent, high-quality AI outputs across your team, using tools you already have. EasySend builds the second: ensuring those outputs flow directly into the systems that need to act on them, without anyone in the middle.
The window is open — but it won't stay that way
The McKinsey and BCG analyses converge on a clear conclusion: insurers pursuing systematic, domain-specific AI integration are already compounding financial and operational advantages. Those persisting with incremental pilots risk structural underperformance that becomes increasingly difficult to reverse.
McKinsey's Insurance Productivity 2030 report projects that more than 90% of pricing and underwriting tasks for personal lines and small commercial products will be fully automated by 2030. The carriers building systematic capability now — structured prompting workflows, documented skill libraries, integrated digital intake — are establishing leads that grow every quarter.
The starting point doesn't need to be complex. Identify the workflow your team finds most time-consuming. Build a structured AI prompt for it. Test it, refine it, share it across your team. Then connect it to a digital intake layer that removes the manual transfer step entirely.
The carriers moving fastest are not the ones with the largest IT budgets. They're the ones with the clearest process thinking and the discipline to act on it.
See how EasySend fits into your operation →