EasySend for Healthcare


































Why healthcare organizations love EasySend
Launch digital journeys
Digitize patient data intake
Save time and resources
Empower your patients
Our suite of
digital products
Create digital journeys for everyone
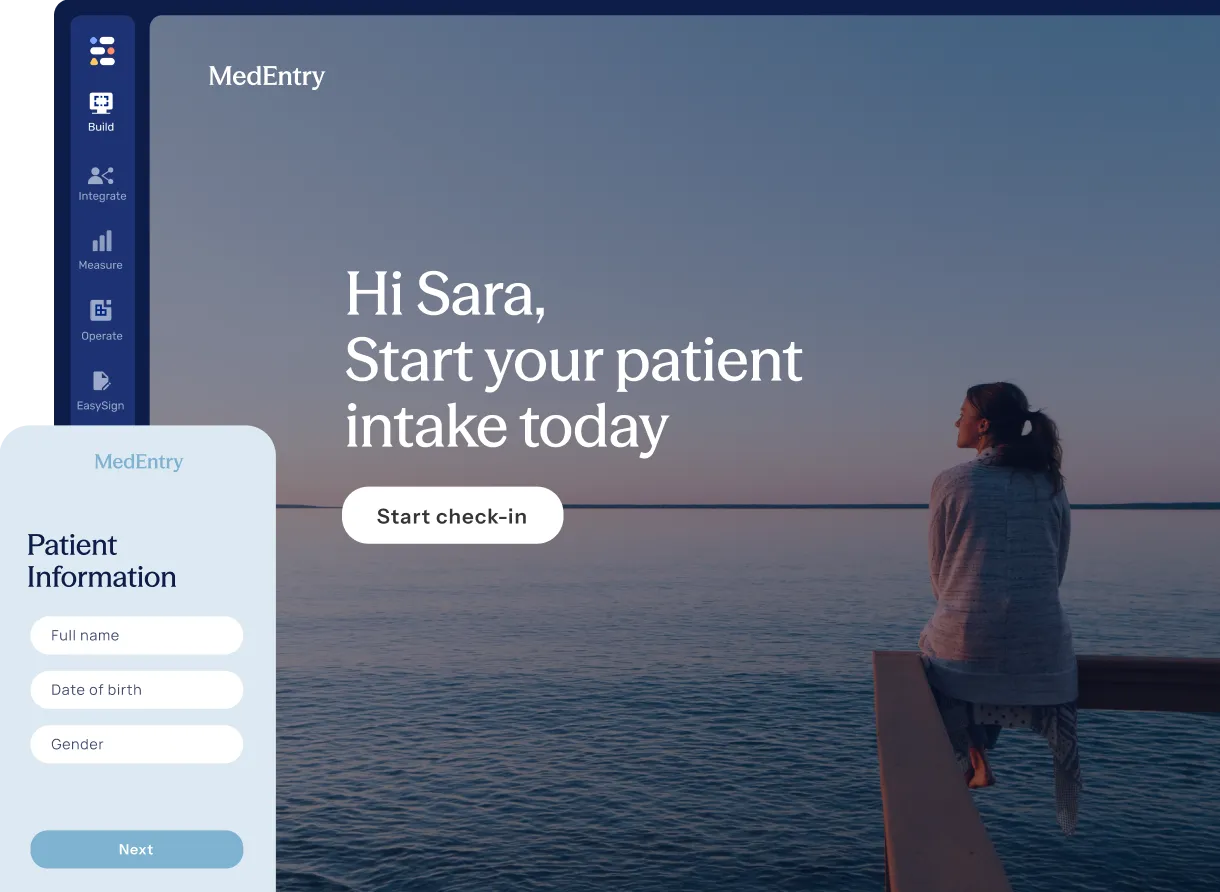
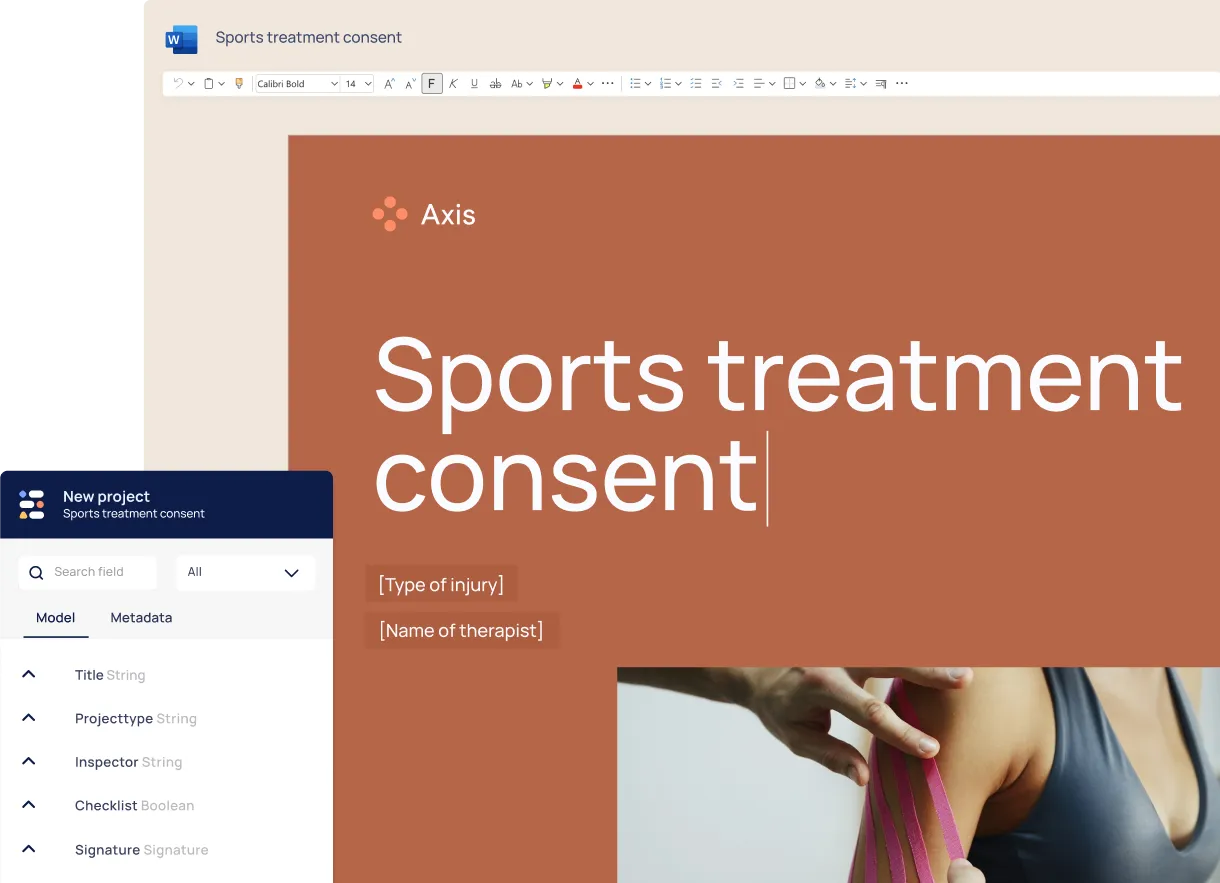
Generate personalized health documents
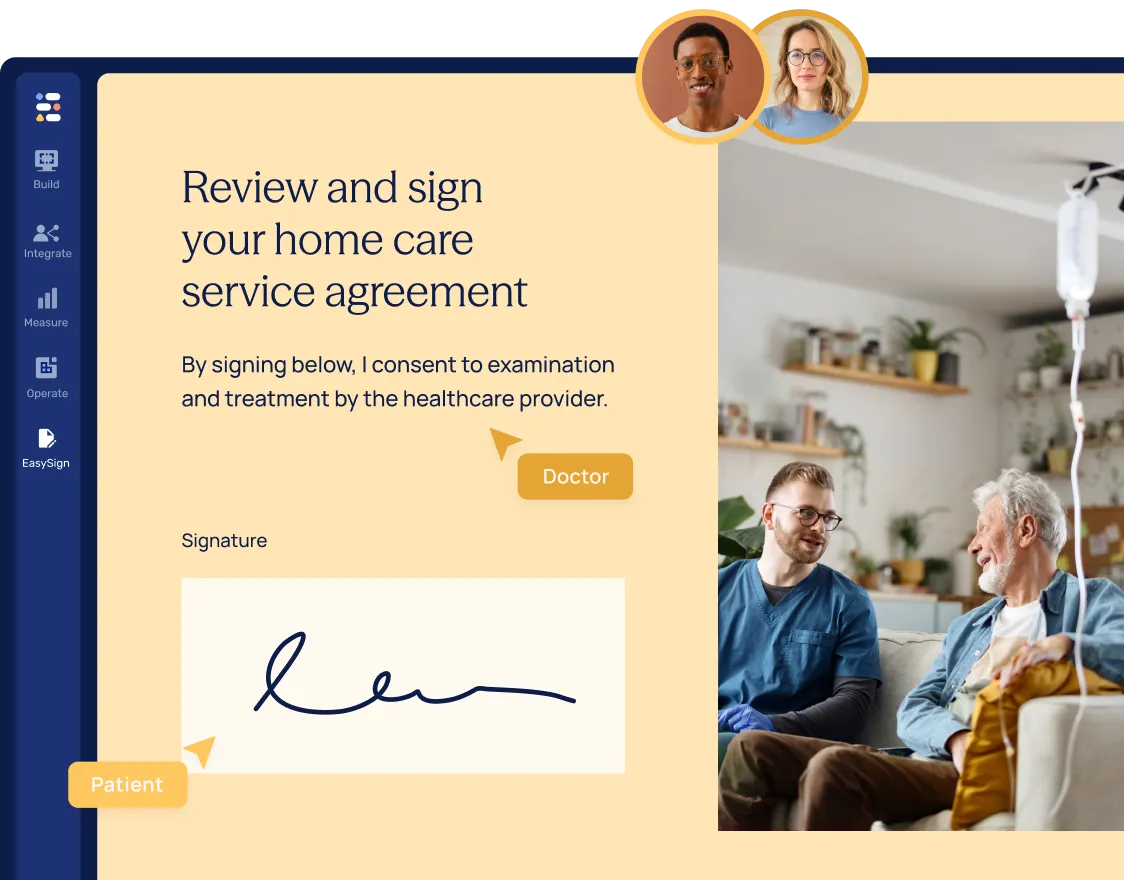
Accelerate patient intake & consent with eSignatures

Map & manage every customer touchpoint
Make data-backed decisions
Elevate your Salesforce workflow



Create patient-centric experiences
Integrate your CRM or ERP to intake patient data and prefill journeys.
multilingual
Speak your customers’ language and support them across any channel.
Upload documents or images, saving all the back and forth.
Create digital interactions that feel native to your brand.
Give customers the ability to complete digital interactions from desktop or mobile.
Enhance your digital journeys with dynamic conditions and smart validations.
Connect your go-to software
Sync your systems in a heartbeat









Protect your patients with HIPAA compliance
We’re committed to protecting your data secure with enterprise-grade security standards. Our platform and electronic signature tool are compliant with the highest international standards, including GDPR, SOC 2 Type II, ISO 27001, PCI DSS, and HIPAA compliance.







